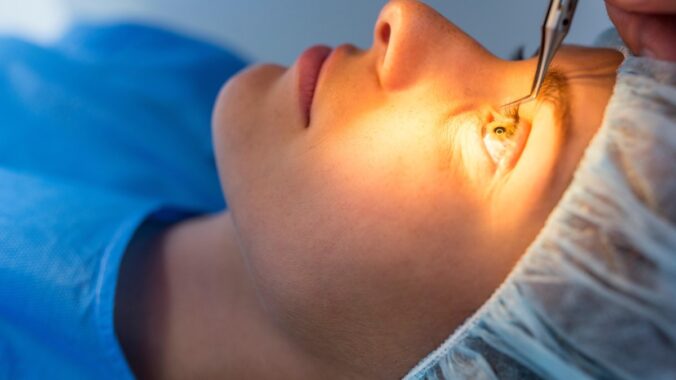
The laser assisted in situ keratomileusis (LASIK) surgery is the safest, most successful, and most well studied elective procedure in the world. It also has the best patient satisfaction rate of any elective procedure that is now available in modern medicine.
If you’ve spent the majority of your life wearing glasses or contacts, there’s a good chance you’ve thought about getting eye surgery LASIK and have been doing extensive study on the procedure.
During the course of your investigation, you have probably come across internet articles and posts on social media that warn of the potential difficulties of LASIK surgery and sensationalise the potential downsides, side effects, and unfounded figures associated with the procedure.
There is sufficient disinformation to cause anyone who is considering treatment to reassess their options and come to terms with the fact that they will need to wear glasses or contact lenses for the rest of their lives.
This happens frequently without ever having consulted with an actual trained ophthalmologist in any capacity.
If they had done so, they would have amassed a plethora of information that, without a shadow of a doubt. It would have given them the ability to make an assured and well-informed decision about whether or not to investigate LASIK eye treatment further.
LASIK Reports of Success and Contentment
There have been literally thousands of clinical studies that have been peer-reviewed and focused on patient satisfaction and visual acuity in relation to the eye surgery of LASIK up until this point.
Since the FDA first gave its blessing to eye surgery with LASIK in 1999, the procedure has undergone significant development. According to additional research carried out by the FDA, LASIK surgery has achieved great success and satisfaction rates.
Furthermore, recent assessments of the literature from throughout the world discovered the following facts:
- Over ninety percent of patients achieve eyesight of 20/20 or greater.
- More than 99% of patients achieve vision that is at least 20/40 or superior.
- There was a 95% satisfaction rate among patients.
- Patients undergoing LASIK eye surgery did not show an increase in the overall prevalence of visual complaints such as starbursts, halos, glare, or ghosting.
LASIK eye surgery has been in use for more than fifteen years, and in Australia alone, it has been carried out more than nineteen million times. When compared to wearing contact lenses for a person’s entire life, statistics show that LASIK eye surgery patients have a far lower risk of experiencing substantial vision loss.
LASIK surgery has the best patient satisfaction rate of any other elective operation; nonetheless, if it were unsafe in any way, this simply would not be the case.
Qualified Surgeons and Eligible Candidates for LASIK Surgery
Although the technology that underpins the eye surgery of LASIK is exceptionally precise and exact, the outcome of the surgery itself is highly dependent on the surgeon who performs it. When contemplating a LASIK eye surgery, it cannot be emphasised enough to search for a refractive specialist that possesses a very high level of expertise.
To become an experienced ophthalmologist who is adept in providing vision correction treatments calls for a significant investment of both time and effort. to prove that they are worthy of the trust that is placed in them to act in a manner that is beneficial to you and your goal.
At our Vision Centers, the process of assessing LASIK eye surgery candidates and determining who is not a candidate for the procedure is extremely crucial. About half of the time, our medical professionals decline the surgery or offer an alternative solution.
A patient who is a suitable candidate for LASIK surgery has an extremely low risk of experiencing a complication. This is especially true when the patient is thoroughly examined and treated by a professional and experienced surgeon with the appropriate equipment.
In addition, prior to surgery, we subject individuals who have previously been authorised to two hours of preoperative testing. Our medical staff does everything in their power to ensure that patients are informed of the potential dangers, taking into account each person’s unique circumstances.
We ensure that our patients are aware of any risk, regardless of how unlikely it may be by utilising a consent form and informative videos.
LASIK Surgeons Put Their Confidence in the Procedure
Ophthalmologists and laser eye surgeons have such a high level of confidence in the LASIK eye surgery that they choose to have it performed on themselves.
Surgeons who specialise in eye surgery with LASIK are five times more likely to have the process done on themselves than the general population, and more than ninety percent of surgeons have either advised or performed this laser eye treatment on a member of their immediate family.
One of the most trustworthy pieces of advice that can be given to a patient who is going to have LASIK surgery is to find a surgeon who has been in the patient’s shoes and been through the operation that the surgeon will be performing on them.
Exceptional Professionals Make Use of Expectations LASIK
Laser eye treatment has been performed on a large scale on members of the general public for many years. Thanks to recent technological advancements, the procedure is now highly qualified to meet the exceptionally rigorous requirements of high-level positions in the Australian military, law enforcement agencies, and professional athletics.
LASIK eye surgery makes use of computer-controlled lasers for eye treatment, which are so accurate and dependable that they meet the stringent criteria necessary for NASA astronauts to undergo the procedure in order to maintain the level of visual acuity essential for them to do their duties.
LASIK of the Highest Quality, Performed by the Best
If you have nearsightedness, farsightedness, or astigmatism, the highly qualified and experienced eye specialists at Personal Eyes are able to effectively and precisely correct your vision, no matter which condition you suffer from.
Lastly
If you are having any question or inquiry about how to have a correct vision, Laser eye surgery, Corneal tissue problems, Lasik surgery, laser beam in healing process, excimer laser usage, refractive eye surgery, laser treatment, laser suite, contact sports, the surgical procedure for refractive surgery or Lasik laser eye surgery – you should get in touch with us via our Personal Eyes website to book your free assessment today.
Related: Understanding the Causes, Symptoms, and treatment of Dry Eyes after Cataract Surgery